The Culture of Fear: And Why You Shouldn’t Take Part
This video explores how the media can create fear which worsens chronic fatigue. This even includes media in the realm of functional medicine, supposedly designed to promote health.

This video explores how the media can create fear which worsens chronic fatigue. This even includes media in the realm of functional medicine, supposedly designed to promote health.

Emotions seem to play a key role in Chronic Fatigue Syndrome (CFS).
This has long been recognised by the wider community of those with the condition, which explains the popularity of mind-body practices to aid with recovery.
This blog looks at a study published in the journal Psychophysiology, which supports this conclusion. The study raises crucial questions about how individuals with CFS experience and communicate their emotions.
The research team compared emotional processing and expression in a group with CFS to a healthy control group, offering valuable insights into this often-overlooked aspect of the condition.
Unveiling the Emotional Landscape:
The study employed a two-pronged approach to explore the emotional landscape of CFS. Firstly, researchers assessed self-reported emotional experiences through questionnaires. This method allowed individuals with CFS to directly report their levels of various emotions, such as anxiety and sadness.
Beyond Self-Report: Decoding Nonverbal Cues:
Secondly, the study went beyond self-report and incorporated an observer-based approach. This involved trained observers viewing video recordings of both individuals with CFS and healthy controls while they narrated emotionally evocative stories. The observers then rated the intensity and clarity with which each participant expressed their emotions through nonverbal cues like facial expressions and body language.
A Discrepancy Emerges:
The findings revealed an intriguing discrepancy between self-reported emotions and observed expression. Individuals with CFS reported experiencing higher levels of anxiety and sadness compared to the healthy control group. Observers also rated the CFS group as expressing their emotions less intensely and clearly compared to the healthy controls.
This suggests that individuals with CFS may be suppressing their emotions to a greater extent than healthy individuals.
Exploring the Implications
The work of doctors such as John Sarno long ago posited that Chronic Fatigue is deeply connected, and indeed indirectly caused by, an individual’s emotional landscape.
While this study makes no explicit connection between CFS and emotional causation, it certainly shows a fascinating correlation. When combined with the experience of recoverers who have used emotional work to recover, this evidence becomes yet more compelling.

A February 2024 study into Chronic Fatigue Syndrome (CFS) by The National Institute of Neurological Disorders and Strokes found that there were abnormalities in the temporal parietal junction, which is the part of the brain that manages the perception of energy.
This suggests that people with CFS may not be physically restricted by their muscles or cells, as has been previously hypothesised, but that their brains are telling them that they are.
The study also found irregularities in the T-cells of the participants, which suggests that the immune system may be overactive and causing a cascade of symptoms. The “immune cascade” theory is also one of the most prominent explanations for Long Covid.
Learn more by watching this summary:

I want to preface this article by saying that I am someone who has both had and recovered from CFS.
Chronic Fatigue Syndrome (CFS), also known as Myalgic Encephalomyelitis (ME), has long been at the centre of a contentious debate within the medical community. One of the most persistent arguments revolves around whether CFS is purely psychological or if it involves physiological factors. This controversy has led to misconceptions and stigmatisation for those suffering from this debilitating condition. Let’s delve into the heart of this debate, examining the evidence and arguments on both sides.
For years, the notion that CFS is purely psychological has been vigorously disputed. Critics of this view argue that reducing the condition to a psychological disorder trivializes the experiences of those living with CFS and undermines the severity of their symptoms. Additionally, attributing the illness solely to psychological factors has led to inadequate medical treatment and support for patients.
One example of this controversy is the historical labelling of CFS as “Yuppie Flu” in the 1980s, implying that it was a condition primarily afflicting the affluent and implying a psychosomatic origin. This term perpetuated the misconception that CFS was a product of a stressed-out, overworked mind rather than a legitimate medical condition.
Furthermore, research into CFS has been fraught with conflicting findings and interpretations. While some studies have suggested psychological factors such as stress or trauma may contribute to the onset or exacerbation of symptoms, others have pointed to physiological abnormalities such as immune dysfunction, neurological issues, and abnormalities in energy metabolism.
However, amidst this controversy, there is an undeniable reality: some individuals with CFS do experience spontaneous remission or improvement in symptoms over time. This phenomenon has led some to argue that the condition may have a psychological component or that symptoms may be influenced by psychological factors such as stress or mood disorders.
Nevertheless, it’s essential to recognise that CFS is a multifaceted condition with complex underlying factors. Recent research has highlighted the role of neurological abnormalities, including dysregulation of the autonomic nervous system and abnormalities in brain structure and function. Additionally, immune dysfunction and inflammation have been implicated in the pathophysiology of CFS.
Rather than viewing CFS as purely psychological or purely physiological, it’s more accurate to understand it as a complex interplay between neurological, physiological, and psychological factors. This holistic perspective is crucial for developing effective treatments and support strategies for individuals living with CFS.
Learn more by watching the video below.
![Fatigue hero image [compressed] Fatigue hero image [compressed]](https://emptyingthebucket.com/wp-content/uploads/2024/02/Fatigue-hero-image-compressed-1160x665.jpg)
Mistakes are often seen as something negative.
This isn’t really the case though.
When recovering from Chronic Fatigue and other complex chronic conditions, making mistakes is actually essential. Mistakes are, in fact, the very fabric of the scientific method – we try, we fail, we try something different. Without mistakes, we can’t actually progress in situations where the next step isn’t clear.
In this video, I summarise three of the biggest mistakes I made, which allowed me to find better paths to recovery.
![callum-skelton-LaMnXPLz7qc-unsplash (1) [photoutils.com] (2) callum-skelton-LaMnXPLz7qc-unsplash (1) [photoutils.com] (2)](https://emptyingthebucket.com/wp-content/uploads/2024/02/callum-skelton-LaMnXPLz7qc-unsplash-1-photoutils.com-2-1160x665.jpg)
Have you ever felt like an emotion just got stuck in your throat or your chest?
At the level of the nervous system, this could actually be the case, as the way we process emotion is richly connected to the muscles, fibres and sinews in our bodies. This is why stress causes stomaches and anger can lead to symptoms like chronic headaches.
Somatic Experiencing (SE) is a therapeutic model which addresses emotions and trauma not on the rational level or words and thoughts, but on a “somatic level” – or the level of our physiology.
Developed by NASA stress expert Dr. Peter A. Levine, this holistic model of healing is gaining widespread recognition for helping to treat intractable psychoneurological issues, including Chronic Fatigue.
While Chronic Fatigue and similar conditions are not psychological, they could be described as being affected by a complex mixture of psychological, neurological and physical factors. Somatic Experiencing helps to address the psychological and neurological aspects of the condition, which may in turn help the body to better process physical stressors. This was the case with my own recovery, which I’ll also discuss in this post.
At its core, Somatic Experiencing is founded on the premise that traumatic experiences can leave imprints in the body, leading to a dysregulated nervous system. Unlike traditional talk therapy, which primarily focuses on verbal processing, SE emphasizes the importance of bodily sensations and movements in releasing stored trauma energy.
I started to use this technique before I even knew the term for it, as it was included in various mind-body healing courses I took. I have since learnt about the impressive body of work that underpins the approach, spearheaded by Peter Levine in his book “Waking the Tiger”.
The outcomes for me were absolutely incredible. The more I practised, the more I could feel trapped emotion literally shaking its way out of my body.
It was an emotionally taxing period, as I had to confront some of my most uncomfortable feelings, but by doing this I began to notice the last vestiges of my chronic fatigue disappearing.
The idea that emotions are trapped in your body would have seemed nonsensical to me before I got Chronic Fatigue Syndrome, but the condition literally forced me to evaluate every available treatment modality. This meant stepping outside my preexisting beliefs about what made sense and what didn’t.
One of the most powerful emotions I tapped into was anger. The funny thing was that I didn’t actually realise I was angry. In fact, I’m a extremely calm person, but when I focused on various events from my childhood, the anger started erupting.
Importantly, I didn’t just stay in the anger, but used this technique to release the trapped survival stress in my body, literally as if I was running or fighting the objects of my aggression.
I also used Eye movement desensitization and reprocessing (EMDR) to help release these emotions.
Although these techniques may seem somewhat intangible, they are profoundly powerful and can work very quickly. I noticed an impact after just one session.
Somatic Experiencing has garnered attention for its effectiveness in treating various forms of trauma, including but not limited to post-traumatic stress disorder (PTSD), childhood trauma, chronic stress, and chronic fatigue. Research suggests that SE can lead to significant improvements in symptoms such as hyperarousal, dissociation, and emotional dysregulation.
From the perspective of this website, one critical thing to note is that reducing this hyperarousal can take the autonomic nervous system out of “fight, flight or freeze” mode, associated with being the causative factor in chronic fatigue and similar conditions.
Somatic Experiencing transcends the traditional dichotomy of mind and body, recognizing them as interconnected aspects of human experience. By addressing trauma on a somatic level, SE facilitates profound healing and integration, empowering you to reclaim agency over your life.
SE paves the way for profound shifts in consciousness and well-being. As we continue to unravel the mysteries of trauma and resilience, Somatic Experiencing stands as a testament to the incredible nature of the mind-body connection.
To learn more about how Somatic Experiencing can be used to treat chronic conditions such as Chronic Fatigue, visit my course page.

It’s common knowledge that stress contributes to Irritable Bowel Syndrome (IBS), with symptoms such as abdominal pain, bloating, diarrhoea, and constipation making navigating daily life a challenge for many. But what does “stress” actually mean on a practical level?
Do we just need to chill out, or is there something deeper at play?
The underlying mechanism lies in our Enteric Nervous System (ENS), a complex network of nerves that governs the digestive tract. When we experience stress, the ENS becomes hypersensitive, overreacting to even minor triggers, leading to a cascade of IBS symptoms. This is part of what many gut health specialists call the “Gut-brain axis”.
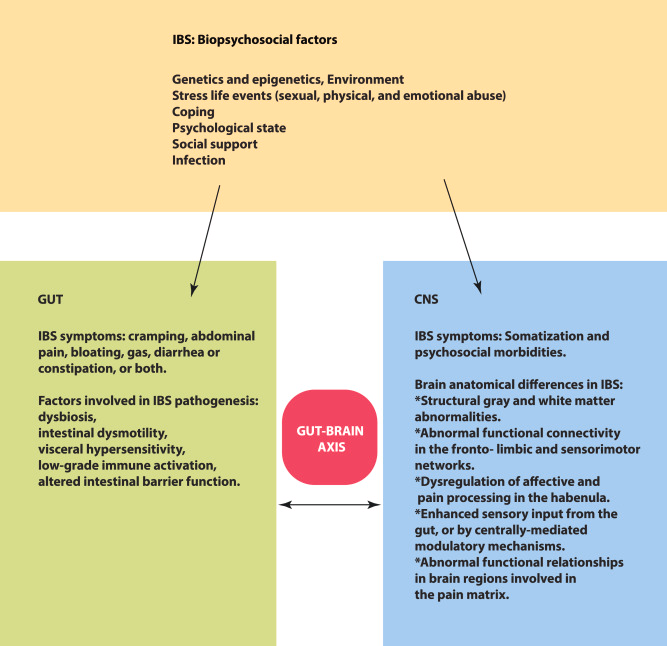
In the diagram below, taken from a study into the effects of hypnotherapy on IBS, you can see how “biopsychosocial factors”, meaning a combination of biological and environmental factors, all contribute to IBS.
These factors dysregulate both the Central Nervous System and your gut, leading to the symptoms we group into the term “Irritable Bowel Syndrome”. While removing one of these factors, such as physical abuse, may help reduce your symptoms, it often isn’t as simple as just removing you from your stressor, as downstream changes have already taken place.
Some of these changes are outlined in the blue box, bottom right, which calls the changes “somatization and psychosocial morbidities”. This idea can simplified by just calling it “changes in your brain and body” due to the initial response to your environment.
One really important takeaway here is that stress isn’t just “stress” in the common use of the term, but “stressors”, meaning infections, lifestyle, life events, genetics, toxins and so on.
The study cited above suggests that stress-induced implicit memories create long-lasting imprints of stressful experiences, which linger in your Enteric Nervous System and can actually alter the expression of your genes. Your environment impacting gene expression in this way is called epigenetics.
Hypnotherapy has emerged as a promising psychological treatment for Irritable Bowel Syndrome (IBS) since the groundbreaking study by Whorwell et al. in 1984. Subsequent research has reinforced the efficacy of hypnosis in alleviating IBS symptoms, prompting a surge of interest in this holistic approach.
Key Findings:

The allure of effortless healing through brain retraining and neuroplasticity techniques has gripped the minds of many seeking relief from chronic conditions like CFS, fibromyalgia, and chronic pain. While these approaches offer tantalising promises of rapid recovery, the reality is far more nuanced.
Testimonials abound, painting a picture of remarkable transformations achieved within weeks or months. However, these testimonials don’t tell the entire story. A significant portion of individuals experience little or no improvement, leaving them questioning the effectiveness of these methods. Those unsuccessful often accuse these programmes of gaslighting them and of raising expectations without any real substance. Others say that if anyone recovers they never had CFS at all, but something less severe.
The key to unlocking the potential of brain retraining lies in understanding that it’s not a one-size-fits-all solution. Individual factors, such as adherence to the programme, compatibility with the brain’s unique makeup, and underlying emotional or subconscious issues, play a crucial role in determining success. It’s possible that some also need to deal with physical issues such as infections before brain retraining can be fully effective.
A holistic approach, encompassing not just brain retraining but also nutrition, lifestyle modifications, emotional release, and subconscious management, offers a more comprehensive and effective path to healing. Integrating alternative practices like acupuncture and vagus nerve stimulation can further enhance the process.
The challenge lies in finding a healthcare provider who possesses a deep understanding of these diverse modalities and can skillfully tailor a personalised healing plan. Neuroplasticity, while a powerful tool, requires patience, perseverance, and a willingness to explore various avenues to achieve lasting improvement.
In the pursuit of healing chronic conditions, a personalised approach coupled with a holistic perspective is essential. By addressing the multifaceted nature of these conditions, people can increase their chances of finding the path that leads to sustainable relief and a renewed sense of well-being.

In this insightful video, hypnotherapist Dana Pycher shares her personal story of how she healed from Chronic Fatigue Syndrome (CFS) and fibromyalgia using hypnosis. She delves into the profound connection between our minds and bodies, explaining how unresolved trauma can manifest as physical ailments.
Pycher introduces the fascinating concept of psychoneuroimmunology (PNI), a way of seeing medicine often discussed by leading doctor and researcher Gabor Mate. It explores the interplay between our emotions, nervous system activity, and immune function. She explains how unresolved emotional distress can disrupt our body’s natural healing mechanisms, leading to chronic health conditions.
To address this intricate relationship, Pycher presents her innovative regression therapy technique. This approach guides individuals back to the root cause of their trauma, allowing them to process and release deep-seated emotional wounds. Through this process, individuals can reclaim their well-being and experience significant improvements in their physical health.
To further illustrate the power of regression therapy, Pycher shares a compelling case study. She recounts the remarkable journey of a client who overcame debilitating fibromyalgia pain using this technique. This real-life example highlights the transformative potential of hypnosis in addressing chronic illness.
Pycher’s video serves as a beacon of hope for individuals struggling with chronic conditions. It demonstrates that our minds hold the key to healing, and that hypnosis can provide a powerful tool for unlocking this potential. By addressing the underlying emotional causes of our physical ailments, we can pave the way for lasting health and well-being.
If you are seeking relief from chronic illness, I encourage you to explore the transformative power of hypnosis. You can embark on a journey of healing that addresses the root causes of your condition and empowers you to reclaim your health.
I’ve created a hypnosis session for you to try for free:

This post summarises a research study into the effect of hypnosis on Chronic Fatigue Syndrome (CFS).
Chronic Fatigue Syndrome (CFS) remains unexplained, but it is characterized by post-exertional malaise – or extreme fatigue which comes on after a period of activity – along with a host of other debilitating symptoms, such as brain fog, impaired circulation, and insomnia.
Even though the extent to which psychology may impact CFS is still hotly disputed, many recovery testimonials mention managing to balance a dysregulated nervous system, so I think this is an avenue well worth further exploration. To add to this wider testimonial evidence of the effectiveness of techniques like hypnosis, I personally used hypnosis extensively in my own recovery from CFS.
The title of the paper I am summarising is : “Hypnosis in Chronic Fatigue Syndrome“, by Vernon H. Gregg, PhD, CPsychol.
The study employed an array of hypnotic techniques:
Three case studies were included:
Case 1: A once-debilitated patient experienced increased activity and social interaction after just 10 weeks.
Case 2: Despite occasional relapses, another patient found surprising control over fatigue and even relief from joint pain.
Case 3: The third patient mentioned is now working full-time with an active social life.
The study does not suggest to me that CFS is a psychological issue, but that hypnosis can contribute to a recovery to different extents. This could be through helping to modulate neurology, the immune system or the Autonomic Nervous System (ANS).